Summer is coming so now is the time to think about your sandals, open footwear, and those beach days ahead of you. For a lot of people, however, the feet they see aren’t anywhere close to being summer-ready.
Discoloration of the toenails and cracked heels are among the top foot-related issues that dermatologists see during the pre-summer time.
Both can result in pain, infection, and other complications — and the good news is that you can heal cracked feet and nail issues easily with the right approach.
In this blog, we will walk you through everything you’ll need to know about treating cracked feet and addressing toenail fungus to get your feet ready for the summer days and your favourite flip flops.
Cracked Heels and Toenail Fungus During Pre-Summers
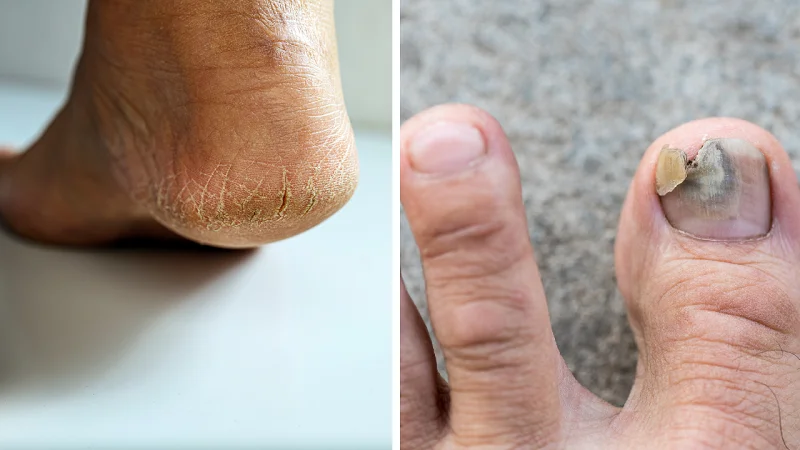
Both cracked heels and toenail fungus seem to occur in the same seasonal pattern; they both tend to spike in the transition from winter to summer. Winter dries out the skin and removes the moisture that your skin needs, whereas the heat and humidity of an Indian summer creates the perfect environment for fungal growth.
Cracked heel fungus treatment is needed when a fungal infection develops in already damaged skin. Dermatologists use urea-based creams, chemical peeling (exfoliating) and in extreme cases, procedural debridement to treat cracked heels.
Toenail fungus is typically treated using anti-fungal medication, topical lacquers and/or laser therapy. Early detection is the best way to avoid extended treatment for both conditions.
Identifying the underlying reason behind why these conditions develop in the first place will help you identify the steps you should take to prevent them. So, let’s explore the main contributors that cause each condition to develop.
Why Do Your Cracked Heels Worsen Before Summer?
Your heels bear a tremendous amount of weight and pressure daily. Moreover, there are some common winter habits that can quietly cause damage to the heels by the time summer comes around. Here are the most common things that contribute to your cracked heels to worsen:
1. Damage Caused by Dry Winter Weather
Dry air steals the natural oil from your skin, including from your heel skin. By the time summer rolls around, months of dryness has already weakened the skin barrier causing it to be more susceptible to cracking.
2. Walking Barefoot Around the House
Walking barefoot on hardwood floors applies direct pressure on the heel pad without providing any protection. The continued pressure of walking on the heel pad over time results in thickened skin which then splits.
3. Dehydration
The first sign of dehydration within the body is often reflected in the skin. If your body does not receive enough water, your skin loses its elasticity.
This loss of elasticity increases the likelihood that the skin on your heel will crack due to the normal pressure that your heel encounters every day.
4. Not Enough Moisturising
Failing to apply a foot moisturizer — especially during the driest months of the year — allows the heel skin to dry out and form callouses. A lot of people also ask themselves, “what deficiency causes cracked heels” Well, know that low levels of vitamin E, vitamin C, zinc and omega-3 fatty acids are associated with poor skin repair and heel dryness.
Severe cases: In extreme cases, if the cracks go deeper than the outer layer of skin, they may become heel fissures. These are painful and can bleed; and if not treated promptly, they may develop an infection.
That you now know how your heels are damaged, you also should know what increases the threat to your toenails in the warmer months.
Why Toenail Fungus Increases in Indian Summers?
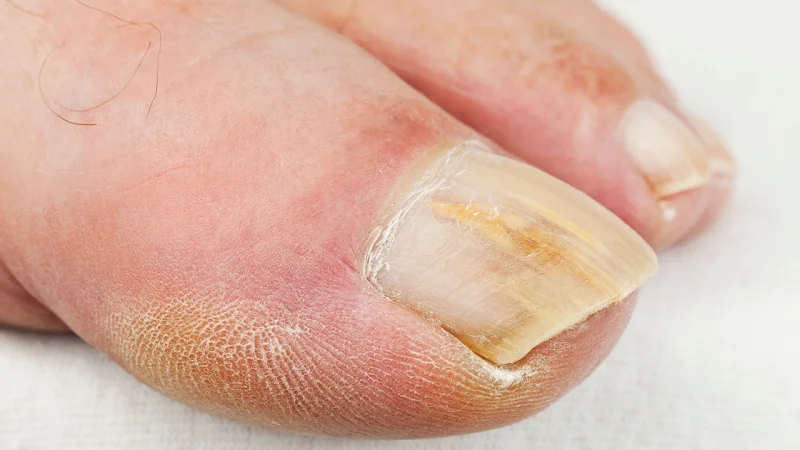
The combination of India’s warm temperatures, the moisture of sweating feet, and the proximity of individuals in public areas create the ideal environment for fungal growth. Several common practices in the warmer months increase your risk of developing a toenail fungal infection.
1. More Sweating
Heat causes the body to sweat more. Sweat creates a warm, wet space between and underneath the toes where fungal spores can grow and infect your nails.
2. Wearing Closed Shoes in Heat
Trapped moisture and reduced airflow to the area around your feet due to wearing shoes that are closed in hot weather provides a perfect environment for fungal spores to colonize in your nail beds.
3. Unclean Salon Equipment
Salon equipment like nail clippers, nail files, and cuticle pushers that are not properly cleaned can spread fungal infections from one client to another. This is especially true as pedicure appointments increase in popularity as summer approaches.
4. Public Swimming Pools and Gym Locker Rooms
Swimming pool wet floors and gym locker room floors are notorious environments for fungi to breed. Even a short period of time walking barefoot on these surfaces increases your chances of contracting a toenail fungal infection.
The sooner you notice a toenail fungal infection, the better chance you have to treat it. Recognizing the early warning signs of a toenail fungal infection will give you a head start on treating it.
Early Signs of Toenail Fungus
In beginning stages, the signs of toenail fungus are not necessarily clinically significant and may be considered by some as cosmetic and non-important. It is only later in time that these changes become more pronounced and obvious to the naked eye and we then realize too late that the fungal infection is severe.
If you are in Patna and see any of the symptoms below, we strongly recommend seeking fungal nail infection treatment in Patna as the longer you leave it untreated, the more difficult it becomes to treat and the more expensive the treatment will become.
Here are the warning signs to look out for:
- Yellowing: The yellowing of a single or multiple toenails is one of the most common indicators of a fungal infection in the toenails.
- Thickening: One of the other key signs that an infection has taken hold is when your nail begins to thicken. Once an infection develops, it can be a lot more difficult to clip your nails as they can become quite thick.
- Brittle nails: If your nails are starting to crumble at the edge and start to snap or break in small pieces when touched, then this is a sure sign that something is wrong.
- Nail lifting: A condition which occurs when the nail starts to separate from the nail bed and the nail then begins to lift, creating a space or gap between the nail plate and the nail bed.
Most people think of dermatology as being to do with just skin cancer and spots. But actually, a skin and nail clinic can offer much more than that, and is actually a far more appropriate place to deal with lots of the common issues we all deal with on a daily basis.
Issues such as nail fungus and cracked heels can be hugely debilitating. But with the right modern dermatological cosmetic treatments and medically-graded products such as those we use in our clinics, these issues can be dealt with quickly and easily.
Dermatological Treatments for Cracked Heels and Toenail Fungus
Over-the-counter treatments for cracked heels and toenail fungus are often ineffective. The skin and nail conditions that cause these problems need to be treated by a dermatologist in order to be resolved.
Once treated, the cracked heels will heal, and the toenail fungus will be completely gone.
Effective Cracked Heels Treatments
The treatment recommended by your dermatologist will depend on the depth of the cracks in your skin. Your dermatologist may recommend or prescribe one or more of the following treatments to correct the condition of your heel.
1. Urea-Based Prescription Creams
Your dermatologist can prescribe creams with high concentrations of urea (20–40%) which have keratolytic effects. These creams help to soften and dissolve the thick skin on the heels, enabling the skin to return to a smooth state without the need for abrasion.
The high viscosity of these creams allows for deeper penetration into the thick hardened skin, leading to quick improvement in the appearance of calluses, even in the most severe cases, in a matter of weeks.
2. Chemical Exfoliation (AHA/BHA Peels)
Application of a dermatologist-strength lactic acid or salicylic acid peel on the heel exfoliates dead skin and effectively repairs the cracks on the skin’s surface.
Another benefit is that it will help soften and even the skin texture on the heel that often thickens into a leathery dead skin. It is almost pain free and you will have to repeat the process a few times for heavily calloused heels.
3. Mechanical Debridement
Dermatologists will use sterile tools to remove the thick hard callus that forms over the skin of the heel.
This treatment works very effectively on deep fissures, as other topical treatments may not penetrate to the full depth. Mechanical debridement can significantly reduce the depth of the cracks. This procedure can be used in conjunction with topical treatments.
4. Occlusive Dressing Therapy
After applying the creams, the dermatologist will apply an occlusive dressing. The occlusive dressing promotes maximum absorption of the active ingredients from the creams.
With deep or bleeding fissures of the heel, occlusive dressing therapy can help accelerate the healing process. It is also highly recommended in the case of fissures that are painful or surrounded by inflamed skin.
5. Platelet-Rich Plasma (PRP) Therapy
PRP is a treatment where concentrated growth factors from the blood are injected into the heel tissue. Growth factors stimulate the skin to heal. Heel fissures that are chronic and non healing after other failed treatments are ideal cases for PRP.
The growth factors stimulate collagen and help restore skin elasticity from within. This will give an obvious improvement in the texture of the skin as well as in the depth of the cracks. However, this improvement can take a few sessions.
Toenail Fungus Dermatological Treatments
The treatment of a toenail fungus is quite time-consuming and a combination of treatments may be required. The treatment that is prescribed by your dermatologist will depend on the severity of the nail involvement and your general health.
1. Oral Antifungal Medications
There are oral medications that can be prescribed by your dermatologist. They include Terbinafine and Itraconazole. These systemic antifungals are considered to be the best treatment for moderate to severe toenail fungus and typically require a 6–12 week course.
The medication is absorbed by the body and travels to the nail bed through the bloodstream where it acts to kill the fungus. It is generally recommended that you have a liver function blood test done for periodic monitoring during the course as a precautionary measure.
2. Topical Antifungal Lacquers
Some dermatologists may recommend medicated nail lacquers such as ciclopirox, amorolfine that can be applied on to the infected nail. These help to curb the growth of fungal infection and are ideal for treating mild fungal infection of the nails or in conjunction with oral antifungal medications.
The nail lacquer may need to be re-applied once or twice a week for several months. The dermatologist will advise on the preparation of the nail surface before application of the nail lacquer.
3. Laser Therapy
Laser therapy delivers a specific amount of light energy under the nail to kill the fungus. It is a safe and effective alternative to oral or topical medications.
Laser therapy works by creating a thermal heat that halts the metabolism of the fungal cells without producing any thermal effect on the nail or the skin. Most patients require 2 to 4 laser therapy sessions, spaced a few weeks apart.
4. Nail Avulsion (Partial or Total)
If the nail plate is heavily infected or is starting to lift from the nail bed, the dermatologist may need to remove the nail partially or totally to allow for optimal antifungal treatment of the nail bed.
Eventually, the nail grows back, and the fungal infection decreases. This procedure is performed under local anaesthetic and is straightforward. Patients are advised that they will need to continue with antifungal treatments until the nail regrows sufficiently to prevent recurrence as the new nail grows back.
5. Iontophoresis-Assisted Antifungal Delivery
Topical therapy is not always adequate for the treatment of fungal infections of the nail. The barrier to penetration, i.e. the nail plate, is thick and inhibits adequate delivery of the topical medication to the site of infection.
Furthermore, there are cases where the nail is so thick that the topical lacquers do not penetrate effectively. Iontophoresis is a technique that uses a mild electrical current to enhance the delivery of the medication deeper into the nail plate.
The process is painless and takes 20–30 minutes. Furthermore, the treatment can be used alongside other antifungal treatments. It enhances drug delivery without the systemic side effects associated with oral antifungals.
The best results are achieved when the treatment is initiated at the optimal time. Early diagnosis and prudent decision to stop self-treatment and seek the expertise of a dermatologist can prevent considerable suffering in the future.
When to See a Dermatologist?
Many people try to treat their own skin problems with at-home remedies or OTC medications for weeks before going to a doctor. While many people’s mild issues will resolve with these solutions, there are some obvious indications that your case requires a medical professional.
If your symptoms persist or get worse, then you should go to a dermatologist sooner than later. Treatment early on does not only decrease the time you have to suffer from your condition, but it also decreases the likelihood of your issue spreading to other areas of your foot or to anyone else in your household.
1. Painful Cracks That Bleed
If your heel fissures crack so deeply that they begin bleeding, then you have a high chance of an infection entering the open area. This is something for which you should seek a dermatologist’s advice right away.
2. Nail Discoloration
If you have been using OTC antifungals for several weeks and you still have a yellow, brown or dark nail, then a dermatologist needs to examine you and give you a prescription for stronger medication.
3. Diabetes Patients with Foot Cracks
As a diabetic, even a small crack on your heel could develop into a major complication. Wounds on a diabetic’s foot take longer to heal and therefore have a greater chance of becoming a deep infection. That is why it is important to be seen by a dermatologist as soon as you notice the signs.
4. Spreading Infection
If you notice your fungal infection is spreading from nail to nail or from your nail to your skin, then you need to see a dermatologist immediately.
Get Your Feet Summer-Ready
Before fungal infections get out of hand, come into our clinic for a dermatological evaluation of your feet. Whatever your issue is — whether it is the nagging crack on your heels or the toenail fungus that just refuses to clear up — delaying treatment only makes things harder for you.
At R Square Skin, Hair, Nail Clinic — recognized as the best skin clinic in Patna — you are in good hands with Dr. Rizwana Barkat (MBBS, MD Skin & V.D), a board-certified dermatologist with years of experience providing dermatologic treatments for heel cracks, heel fissures, and toenail fungus. The treatments are personalized to your skin type and degree of severity.
This summer, let your feet take you wherever you want to go. Give yourself the gift of healthier, happier feet. Schedule your appointment with us at R Square Clinic today.